Introduction
Chronic Kidney Disease (CKD) is one of the most prevalent chronic conditions in feline medicine, particularly in aging cats. A significant and clinically impactful complication of CKD is non-regenerative anemia, which contributes to reduced quality of life, weakness, and increased morbidity.
Understanding and improving the management of CKD-related anemia remains a key focus in veterinary therapeutics.
Pathophysiology of Anemia in CKD
Anemia associated with CKD is multifactorial, with the primary mechanism being:
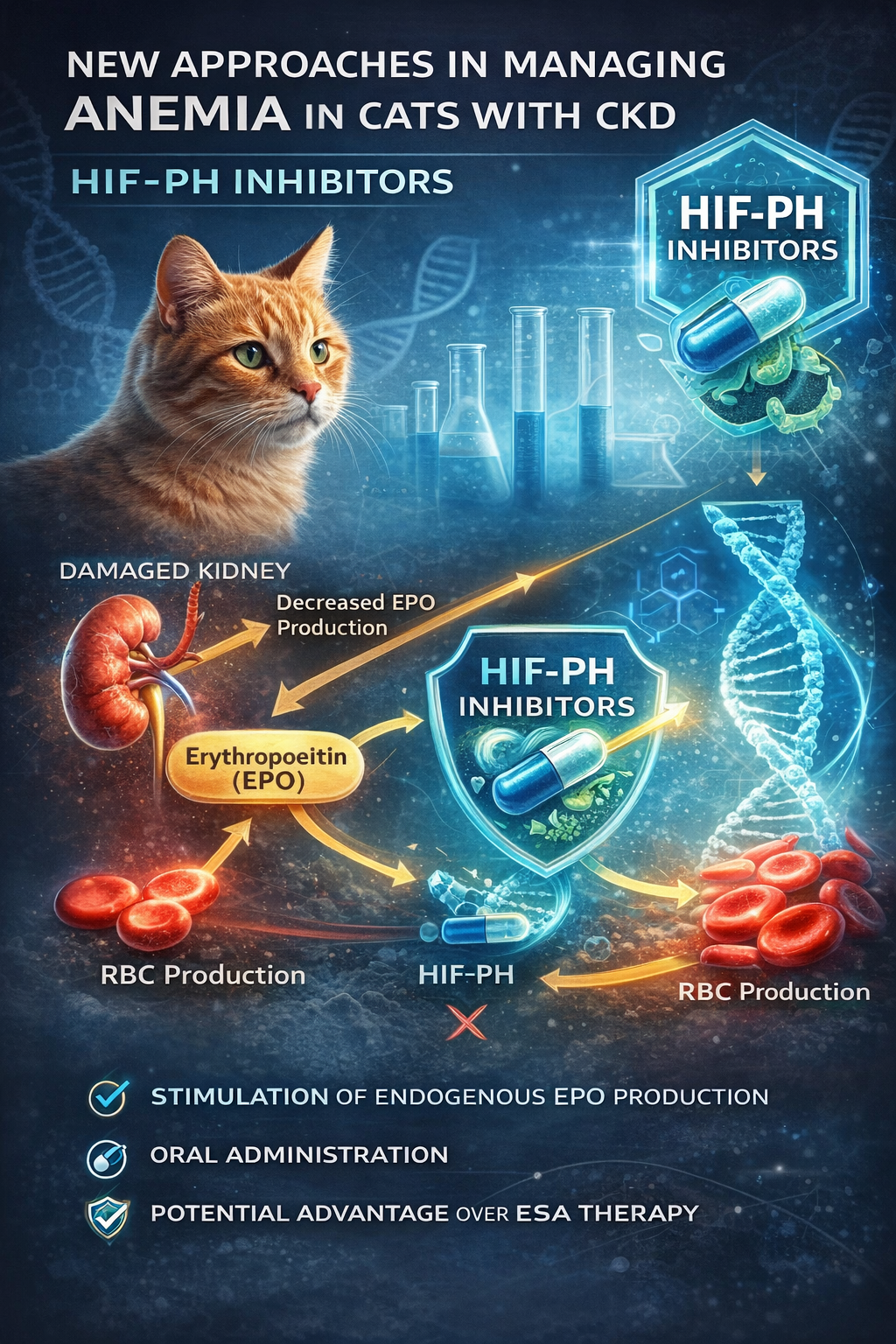
- Decreased production of erythropoietin (EPO) by damaged renal tissue
- Reduced erythropoiesis in the bone marrow
- Shortened red blood cell lifespan
- Chronic inflammation
These factors collectively lead to decreased hematocrit and hemoglobin levels in affected patients.
Limitations of Current Therapies
The current standard of care often involves the use of erythropoiesis-stimulating agents (ESAs) such as epoetin alfa or darbepoetin.
However, several limitations are associated with these therapies:
- Risk of anti-EPO antibody formation
- Variable clinical response
- Requirement for repeated parenteral administration
- Potential immunological complications
These challenges highlight the need for alternative therapeutic approaches.
The HIF Pathway: A Physiological Target
The Hypoxia-Inducible Factor (HIF) pathway plays a central role in the body’s natural response to hypoxia.
Under low oxygen conditions:
- HIF is stabilized
- Transcription of EPO is increased
- Red blood cell production is stimulated
In normoxic conditions, HIF is rapidly degraded by the enzyme:
👉 HIF-Prolyl Hydroxylase (HIF-PH)
Mechanism of HIF-PH Inhibitors
HIF-PH inhibitors represent a novel therapeutic class that:
- Inhibit the activity of HIF-PH
- Stabilize HIF under normoxic conditions
- Promote endogenous (natural) EPO production
This mechanism mimics the body’s physiological response to hypoxia rather than introducing exogenous hormones.
Potential Clinical Benefits
Based on emerging data, HIF-PH inhibition offers several potential advantages:
- Oral administration, improving patient compliance
- Stimulation of endogenous erythropoiesis
- Reduced reliance on injectable therapies
- Potentially lower risk of immunogenic reactions compared to ESAs
Clinical Considerations
When considering this therapeutic approach, clinicians should be aware of:
- The importance of assessing iron status prior to and during therapy
- Monitoring parameters such as:
- Packed Cell Volume (PCV)
- Hematocrit (HCT)
- Hemoglobin levels
Additionally, attention should be given to:
- Blood pressure monitoring
- Risk of thromboembolic events in susceptible patients
Comparative Overview
| Feature | ESA Therapy | HIF-PH Inhibitors |
|---|---|---|
| Mechanism | Exogenous EPO | Endogenous stimulation |
| Administration | Injectable | Oral |
| Immunogenicity | Potential concern | Potentially reduced |
| Physiological alignment | Limited | High |
Clinical Perspective
HIF-PH inhibitors may represent a promising option in:
- CKD-related anemia in cats
- Patients with poor response to ESA therapy
- Cases where injectable treatments reduce compliance
Ongoing research continues to evaluate their role in veterinary medicine.
Conclusion
Targeting the HIF pathway introduces a novel, physiology-based approach to managing anemia in feline CKD.
By stimulating endogenous erythropoietin production, HIF-PH inhibitors may offer:
- Improved safety profile
- Enhanced compliance
- A complementary or alternative strategy to traditional ESA therapy
Discussion Point
How do you see the role of physiological erythropoiesis stimulation evolving in the management of CKD-related anemia in feline patients?
❓ What are the main challenges in managing anemia in cats with CKD?
Anemia in feline CKD is typically non-regenerative and primarily caused by reduced erythropoietin (EPO) production. Common clinical challenges include:
Difficulty maintaining long-term stability
Inadequate response to therapy
Progressive decline in hematocrit
Reduced patient quality of life